
How to best use third-party patient stories to help patients overcome the fear of surgery
Third-party patient stories are one of the best ways to help people overcome their most significant objections to surgery – fear of the unknown being the most significant.
Most people working in elective surgery know that the two most significant barriers to adoption is 1) cost and 2) fear. As I’ve progressed through my career and my personal eye surgery journey, my experience convinces me that one is considerably more significant than the other.
How I know fear is the most significant barrier to more people having laser eye surgery:
As the race to the bottom has proven, price-cutting is not the route to jump-starting eye surgery volumes. For the majority who could benefit from laser eye surgery, even the lowest-price inducements of £399/eye are insufficient. No, the price objection is a superficial smokescreen that masks a deeper objection – fear. Helping people overcome the fear objection, therefore, is one of the most important jobs for anyone offering laser refractive surgery.
The prominence of the third-party patient’s story
What would persuade you more:
- A statistical chart,
- A 5-star review or
- A detailed video or textual account of how someone transformed their life through eye surgery?
All three are great, but one is far more potent than the other.
For most people, third-party stories are more persuasive than praise and statistics because individual examples play into our natural predisposition to remember stories better than numbers and abstract ratings.
Stories are compelling because they can transport us to the journey as it unfolds. Watchers or listeners of a good story can put themselves in the picture and step into other people’s shoes.
The most compelling third-party patient stories position the patient as the hero, with the surgeon as the mentor or guide. You can do this by crafting stories around your patient’s experiences and the Hero’s Journey – including their fears – and featuring them in every way you communicate.
If you’ve ever consumed popular entertainment, the Hero’s Journey will be familiar to you. It’s a well-used story arc that forms the basis of our most famous stories, myths and legends.
How can you use this character arc in written, audio or video patient stories to help your patients motivate themselves? I hope to answer that question in this post. Before we get started, however, understand these crucial points:
- The purpose of a third-party patient story is to elicit emotion. For the story to compel, it must make people feel something, not just think about something
- The three elements of any compelling story are a hero (or protagonist), their desire, and a conflict. In the ‘Hero’s 2 Journeys’, Hollywood story consultant Michael Hauge puts it this way: “Every good story is about a captivating or emotionally involving character who is pursuing some compelling desire and who faces seemingly insurmountable odds in achieving it.”
- Position the patient as the hero of the story (not you, the clinic or the surgeon). You must position yourself as the patient’s mentor or guide. Frame their desire as a life without glasses (not having surgery). Set the conflict as their own fear, or another circumstance that made it extremely difficult for the hero to get what they wanted.
- Consider both the hero’s outer journey (having surgery to get a visible result) and their inner journey (how they are growing and transforming psychologically, emotionally or spiritually as a result of their journey).
The Hero’s Journey in 12 stages
The diagram I’ve included below represents the 12 Stages of the Hero’s Journey. This arc is a popular narrative structure derived from Joseph Campbell’s Monomyth explained in his book “The Hero With A Thousand Faces”1 and adapted by Christopher Vogler in the Twelve Stage Hero’s Journey2.
The reason this metaphor is so commonplace is that it’s worked on us for millennia – across myths and legends of many cultures from ancient to modern times.
There’s something about our brains that implicitly understands and identifies with this all-embracing monomyth. We can’t help but be compelled by it, despite its ceaseless repetition across all forms of storytelling – in film, in games, in literature and television.
Writers have used The Hero’s Journey for centuries because it works. You too can make it work for you. In the post that follows, I’ll frame my third-party patient story using the stages of the Hero’s Journey so that you can see how you can help frame any patient’s story into a compelling tale that will inspire other prospective patients.
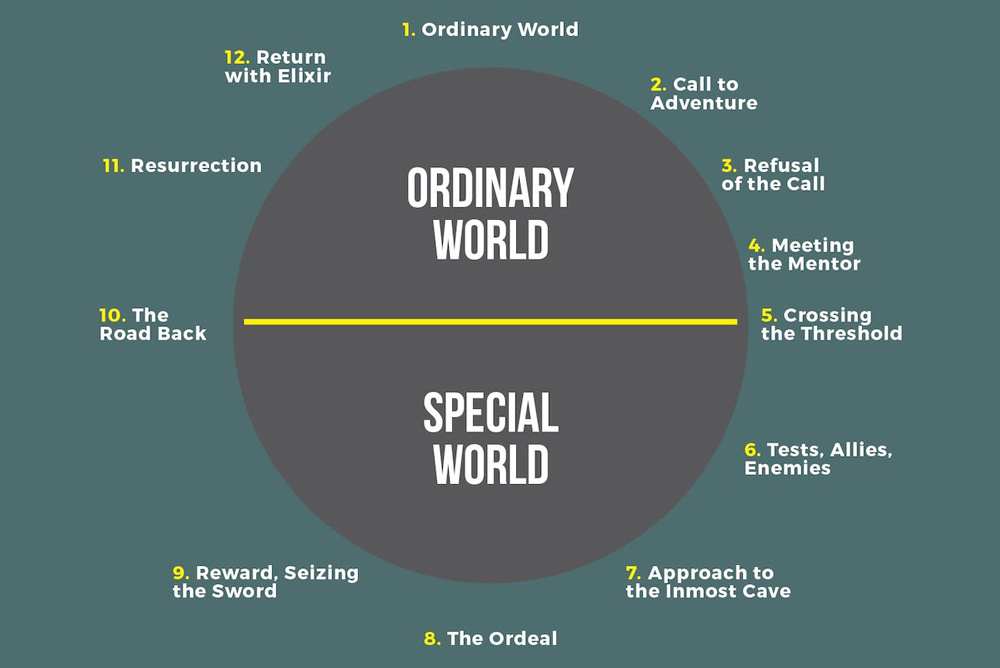
The 12 Stages of the Hero’s Journey diagram.
1. The ordinary world
This is the time for surgeons to understand their patients before-state.
- What do they have and feel before surgery?
- What’s their average day like?
- What’s their status? (How do they imagine others see them?)
- How do they see themselves concerning how life is and how it ought to be?
When structuring your third-party patient story, ensure you introduce your hero while they’re in the ordinary world by enabling your audience to empathise with their challenges before their transformation. I advise marketers to do this in awareness marketing, regardless of channel (search, social, direct, and broadcast). The goal is to present your hero as someone with whom people can empathise. They must become the hero and identify with them. We want them to experience the same emotions with the hero.
How? Hauge advises you to make the hero identifiable by employing two or more of the following elements when introducing the hero:
- Make the audience feel sympathy for the hero by showing them as the victim of some undeserved misfortune
- Highlight how the hero is in jeopardy
- Show the hero’s likeable side. Highlight how they are a kind-hearted or good person. Show how others like them.
- Show the hero’s funny side. If they have a sense of humour, put it on display. We like people that make us laugh and have the courage to take risks and say funny things where we may not.
- Show the hero’s power or ability. Show how they are good at what they do. We admire, are attracted by and want to become people who have extraordinary abilities or previous successes.
This stage is your opportunity to help your audience identify with your patient avatar’s ‘drives, urges and problems’. This is the hero’s – your patient’s – before state – or their ordinary world. Their growth and transformation can only occur when they leave the ordinary world and start on the often scary path towards the special world – out of their comfort zone and into discomfort.

2. Call to adventure
At this stage, you must put your patient’s problem on display and show how their call to adventure gets the story rolling because it throws their ordinary world off-balance. Your patients do not seek surgery at this stage; instead, they seek transformation to an after-state. Surgery is only a possible vehicle towards an after-state.
This stage is your opportunity to show the appeal to the adventure of the after-state – a special world free of spectacles. For example, after-states could be freedom from glasses, an enhancement of ability, and the expansion of opportunity. These types of appeals are significantly more persuasive than the more common self-centred branding, claims of superior expertise and technology, or inducements to save money that we see most in health advertising.
Know that it’s normal for a hero to need a succession of calls before finally realising that their challenge must be met. Interview the patient to find out what their call to action was, and if and how they at first refused the call.
3. Refusal of the call
Refusing the call is normal. Expect it and work help your patients to overcome it. Feature it in your third-party patient’s story.
Framing the outer journey to a life without glasses as a personal growth experience is fundamental. Every modern day hero – from Luke Skywalker to Wonder Woman to Frodo Baggins to Alien’s Ellen Ripley to Neo in the Matrix – when starting their journey of transformation experienced fear. Often, that fear is of the unknown. Feeling the fear and doing it anyway5 is the only way they moved forward and grew as a result.
Think about every Hollywood movie you’ve watched. The refusal of the call is an essential stage of the journey. As Vogler says: “Without risks and danger or the likelihood of failure, the audience will not be compelled to be a part of the Hero’s Journey.” A dramatic story demands stakes. If the patient does not experience any perceived threat or danger, the story loses interest.
It’s now worth taking a moment to discuss patient fear and how to overcome it.
If you want to help your patients overcome their fears and assume that if you can only inform them enough; that knowledge alone is sufficient to dispel their fear – you’re partly right. Because fear is often irrational, however, cold-hard rationality alone isn’t enough to help a person overcome their fears.
You have to acknowledge – loudly and clearly – that their fears are real, that what they feel is normal and legitimate, and that you can help them overcome their fears. Crucially, however, taking action – no matter how small3 – is a mandatory pre-requisite to overcoming fear. The more options you can give your patients to make these micro-commitments, the more opportunities you’ll give them to overcome fear with action.
In your third-party patient story, show how the hero took these micro-commitments and how their action led to the eventual erosion of their fears.
Fear is common in anything new (not new to you, but new to a patient). Fear in people will never go away as long as they continue to grow or cope with changes in their environment. Susan Jeffers4, a psychologist who devoted her career to understanding fear and how to overcome it, said:
“Every time you take a step into the unknown, you experience fear. There is no point in saying, ‘When I am no longer afraid, then I will do it.’ You’ll be waiting for a long time. The fear is part of the package.”
(NOTE: Want to see how your practice marketing measures up against the best in class? Take this 5-minute quiz to see how you stack up in the 9 areas of practice marketing and get specific tips and advice on how you can improve your weak points and better leverage your strengths).
4. Meeting the mentor(s)
The only way for patients to overcome the fear of doing something is to do the thing that scares them. Jeffers adds:
“When you do it often enough, you will no longer be afraid in that particular situation. You will have faced the unknown and you will have handled it. Then new challenges await you, which certainly add to the excitement in living.”
The idea of feeling the fear and doing it anyway5 is the basis of systematic desensitisation, a well-proven treatment of phobias. This therapy aims to remove the fear response of a phobia by systematically exposing the anxious subject to more anxiety-producing stimuli of the thing that induces fear and substituting a relaxation response to the conditional stimulus gradually using counter conditioning.
- Rewarding patients for their demonstrated courage in booking the first appointment can help them to remain consistent with their prior actions and keep their scheduled appointments.
- For many patients, merely walking into a clinic where surgery is performed will cause anxiety. Initiating a warm welcome call a week before to let them know you’re eager to see them and calm their worries (buyer’s remorse) serves to reduce DNA rates.
- Meeting the mentor (that is, the surgeon – or an extremely credible optometrist) is crucial. Importantly, the mentor needs to demonstrate their authority to guide the patient, providing a map and the empathy the patient requires to submit to their instructions.
Many clinics seek to save time and costs so they skip these steps. I feel that’s an error for various reasons – number one is that the patient fails to meet the mentor who helps them get over their fear (ergo, more delay and more declines).
5. Crossing the threshold
At first calls and appointments, seek to identify what the patient fears explicitly. As an exercise, ask them to rank the aspects of the surgery that causes them to be anxious.
Give them, or direct them to, a resource to help them learn simple relaxation or coping techniques such as meditation, tensing and relaxing parts of the body (progressive muscle relaxation), and breathing exercises. Many smartwatches, like the Fitbit and the Apple iWatch, have built-in relaxation routines patients could use. YouTube is full of videos that demonstrate and guide people through meditation, progressive relaxation and stress management approaches.
Understand that many patients feel like crossing the threshold is a liberation of sorts. They’ve finally made a commitment, taken a risk in even showing up, and begin to anticipate the resolution of their problems with excitement and positivity. Take advantage of this state to show the patient that you can measure up to their expectations of a mentor who can confidently lead them towards the conclusion of their journey.

6. Tests, allies and enemies
Systematically expose prospective patients to what they fear (from least to most) and have them connect the successful coping mechanism with each increasingly fear-inducing stimulus. For example:
- Calling some of your measurements “test-drives” for those who fear people touching their eyes can help.
- Guiding patients into the surgical suite and asking them to relax on the treatment bed might be useful to help the anxious cope with the unknown.
You don’t need to be a trained psychologist to carry out these techniques. Many people, myself included, practice approaches to calm themselves in the face of fears to successfully transcend them. For example, I have a little ritual I practice whenever I’m about to lift a weight I feel is a new challenge: I will typically silently mouth the words “I can do this” and then proceed to do it. When I’m about to throw myself down a challenging hill on my snowboard, I’ll similarly clap my gloves together two or three times before I lean into it.
After the initial period of optimism generated by simply crossing the threshold, the patient needs to acclimatise to the special (clinical) world. These can include inconveniences like:
- Sitting idly in a waiting room without much to do but worry,
- Waiting much longer than is seemingly necessary,
- Overhearing reception and clinical staff carry-on about trivial pursuits,
- And generally, feel like a stranger in a strange land.
This stage is an opportunity for your staff to position themselves as the hero’s team – like a Fellowship to Frodo, Luke’s fellow rebels aboard the Millennium Falcon, or Neo’s crew-mates on the Nebuchadnezzar. Everything the patient sees “on-stage” should feel to them like it’s designed to help them on their journey. If it doesn’t, stop the behaviour and move it “off-stage”, out of the patient’s scope of observation.
Your front desk staff’s number one job at initial appointments is to ease the patient’s tension, focus on their comfort, reduce their anxieties and ensure they are kept abreast of what to expect – especially when things change from the expected norm.
Patient liaisons must assume the role of an ally, walking alongside the patient on their first appointment pathway, introducing them to the other allies and mentors along the way.
Hero’s often have an ultimate sidekick they can trust, which is why I always encourage you to invite your patient’s significant others to travel alongside them on their journey. Having a friend or family member accompany the patient into theatre might seem like a needless inconvenience (especially if they’re anxious themselves!). Still, it can help an anxious patient feel a sense of familiarity in unfamiliar surroundings.
7. Approach to the inmost cave
The big day has arrived and your patient, accompanied by their ally, have made their way to your practice. At this stage, don’t underestimate the soothing power or human touch. A permitted touch on the shoulder can go a long way to reassure someone who is anxious.
A designed-for-purpose room complete with dim lighting, essential oils and a head and shoulder massage from a massage therapist, is a wonderful extra touch that can go a really long way in relaxing your patient and making their experience a pleasant one.
8. The ordeal
The Ordeal in any hero’s journey is sometimes a dangerous physical test or a deep inner crisis that the hero must face to survive or for the world in which the hero lives to continue to exist.
As nearly everyone who’s had laser eye surgery knows, the imagined ordeal is significantly more terrifying than the event itself:
This is, of course, the main event. For most, it’s over before they know it.
If you want to make their experience even more comfortable, provide them with:
- A plush toy to hold onto during the surgery can help to alleviate patients common anxiety symptoms such as muscle tenseness, trembling and sweating.
- A heavy blanket can help to keep the patient warm in what is often a cool room and prevents them from reflexively lapsing into self-protection mode by bringing their hands up to their face in a panic.
- The magically reassuring power of well-timed words can make the patient feel like they’re doing everything right while doing nothing but lying there like a stone.
- A need to know basis (the empty silence is scary)! Informing the patient of everything they need to know, only a moment before it happens, irradiates any doubt that may be in their mind.
9. Reward
The surgery is now complete. With LASIK, patients typically experience the “Wow Effect”. It’s a powerful moment that you should help celebrate.
It can be an emotional experience for many. The sense of relief (it worked!) is palpable and reinforced at that moment. You want to make your patient feel like King Arthur who’s just pulled Excalibur from the Stone.
10. The road back
The road back can be so much more than post-op visits. Imagine different ways to celebrate your patient’s return to their ordinary world to keep it as special as possible. Recognition, token gifts or cards, follow-up calls in between appointments, all can help to lend your hero assistance as they recover from their ordeal.
11. Resurrection
According to Jeffers:
“This is the one truth that some people have difficulty understanding. When you push through the fear, you will feel such a sense of relief as your feeling of helplessness subsides. You will wonder why you did not take action sooner. You will become more and more aware that you can truly handle anything that life hands you.”
Patients want to be understood and empathised with. They need their guide (that is, their surgeon or clinic) to appreciate what they have, how they feel, what their daily life is like, and their status before they guide them to where they want to go.
Most importantly, they don’t want their surgeon or their clinic to be the hero. That’s not an effective way to calm their fears. They already expect the surgeon to be fearless. They, the patient, must overcome their own anxieties and transform into the hero and protagonist of the story, with the aid of the guide.
12. Return with the elixir
The patient will return with an elixir of clarity, destined to bring hope to those they left behind, re-convinced of a direct solution to their problems and a fresh perspective for you – the readers – to consider.
Jeffers says:
“This should be a relief. You are not the only one out there feeling fear. Everyone feels fear when taking a step into the unknown. Yes, all those people who have succeeded in doing what they have wanted to do in life have felt the fear – and did it anyway. So can you!”
This truth relies on social proof, which is a psychological phenomenon where people assume the actions of others in an attempt to reflect correct behaviour for a given situation.
One of the worst things you can do is to tell people that they shouldn’t be afraid, or that they’re alone in their fear. In truth, most people are fearful of eye surgery, and that’s OK!
People assume many coping strategies to assuage their fears through social proof. For example, one of the primary reasons people look at reviews before making a purchase is because they are anxious to know how others experienced and overcame their fears.
When soliciting reviews, I advise prompting your patients to cite their fears and how they overcame them before surgery as the central theme of their reviews. For example, when asking for reviews, ask the happy patient:
- What are the problems you experienced before you discovered what you could do about your eye problem?
- What did you want to do or accomplish after surgery? (What was your call to adventure?)
- Did you at first refuse the call? If so, why, and for how long?
- What frustrations did you experience when trying to solve your problem?
- What’s different about dealing with us compared to others you tried?
- Take me to the moment when you realised that the treatment worked?
- Tell me what life looks like now that you’ve solved or are solving your problem?
- What would you tell someone who was scared about eye surgery?
Social proof is powerful. One study, cited in the Washington Post, even showed how positive social proof can be more influential than saving money.
(NOTE: Want to see how your practice marketing measures up against the best in class? Take this 5-minute quiz to see how you stack up in the 9 areas of practice marketing and get specific tips and advice on how you can improve your weak points and better leverage your strengths).
12 ways you can use the hero’s journey stories in your marketing
- In your awareness and engagement marketing, show your patients you understand their “ordinary world” challenges and show them how life could be after they heroically make the first move away from their comfort zone. Speak to the fear directly in:
- Advertising campaigns
- Social media posts
- E-mail marketing
- Blog posts
- Lead magnets like guides
- Infographics
- Media for publicity
- On your website’s homepage. Using video or text, show the would-be hero’s adventurous life without glasses. Feature people they can identify with enjoying all the things they can do after completing their journey.
- In your telephone calls. Help callers understand how others similar to them experienced fear of “crossing the threshold” and overcame their fears by booking an appointment. Have your telephone handlers memorise archetypical patient stories so they can share them using an abridged form of the Hero’s Journey.
- In your consultations, where your patients “meet their mentors”, imagine all the ways you can help your patients feel like heroes. I’ve suggested several action points above.
- In seminars and webinars. These events are most compelling when a patient shows up to directly share their hero’s journey. Help them tell it by crafting slideshows for them to present that follow the Hero’s Journey.
- In video testimonials, interview your patients in such a way that they answer questions that help them share their third-party patient story in the Hero’s Journey format.
If you want to know how I became The Hero and conquered my fear of laser eye surgery, stay tuned for my next blog post where I will include the video of the full 16-minute laser eye surgery operation in real-time from start to finish.
(NOTE: Want to see how your practice marketing measures up against the best in class? Take this 5-minute quiz to see how you stack up in the 9 areas of practice marketing and get specific tips and advice on how you can improve your weak points and better leverage your strengths).
About the author

Rod Solar
Founder & Scalable Business Advisor / fCMO
Rod Solar is a co-founder of LiveseySolar and a Scalable Business Advisor for its customers. Rod mentors and coaches eye surgery business CEOs/Founders and their leadership teams to triple their sales, double their profit, and achieve their “ideal exit”.
Related Posts
Meet our Co-Founders

Rod Solar
Founder & Scalable Business Advisor
For over 20 years, I’ve helped ophthalmology entrepreneurs scale their private practices. I specialise in doubling revenue within three years by offering a proven framework, hands-on experience, and a team of experts who implement what works. We take the guesswork out of growth and scale, so you can focus on delivering exceptional patient care while maximising the value of your business.
LiveseySolar completely transformed the way we were approaching this… We’ve gone from having just the dream of having a practice to having a practice up and running with people making inquiries and booking for procedures… It’s extremely pleasing. We feel lucky we connected with LiveseySolar.
— Dr Matthew Russell, MBChB, FRANZCO, specialist ophthalmic surgeon and founder of VSON and OKKO

Laura Livesey
Founder & CEO
I’m the co-founder & CEO of LiveseySolar. I’ve developed powerful eye surgery marketing systems that increase patient volumes and profits for doctors, clinics, and hospitals, since 1997.
Rod and Laura know as much about marketing surgery to patients as I know about performing it. They are an expert in the field of laser eye surgery marketing. They know this industry inside out. I believe that they could help many companies in a variety of areas including marketing materials, sales training and marketing support for doctors.
— Prof. Dan Reinstein, MD MA FRSC DABO, founder of the London Vision Clinic, UK









